Contraceptives, informally known as birth control, can help prevent pregnancy when you aren’t ready for or don’t want to have children. When you’re considering which contraceptive is “right” or “best,” remember that there is no one-size-fits-all method. Any type of birth control has its upsides and downsides, depending on the user. Some methods also provide additional benefits or alternative uses.
It’s important to learn more about the types of birth control, whether you’re looking to switch or have minimal experience. You can then consider your own personal goals, the contraceptive’s degree of effectiveness, and how convenient or inconvenient it is for you so you can make an informed decision. We’ve compiled this information about the various methods of birth control, how to determine what could be ideal for you, common misconceptions, and more.
Factors to Consider when Choosing a Contraceptive Method
The first factor most people must consider when choosing a birth control method is accessibility; how accessible are the various methods for you? Will your insurance cover birth control, or is there a copay? Are you able to get it at your local drugstore or the pharmacy, or is a medical professional needed? After you’ve identified a list of affordable options or those covered by insurance, it’s important to consider a few other factors to narrow the list to the best birth control for you.
Your Lifestyle and Preferences Can Influence What Works for You
Your lifestyle has a significant role to play in your birth control choice. For example, if you don’t have sex often, you may be fine relying on condoms since they’re affordable, and you won’t need to replenish your supply often. Alternatively, if you live a busy lifestyle but have sex a bit more often, you might want to consider hormonal birth control; while some forms of hormonal birth control need to be picked up on a regular basis, they can provide consistent protection. As a result, there’s no need to plan or worry about having unprotected sex if your method has constant coverage and only a monthly pick-up.
It should be noted that all forms of birth control can only be at their peak effectiveness when used correctly. For that reason, a critical question to ask yourself is whether you will be able to use it correctly as is required every time. Some hormonal contraceptives take a bit more effort to use as instructed. For example, the Pill, which needs to be taken daily, may be more difficult for busy or forgetful individuals to take correctly. For those individuals, condoms or an IUD may be more viable options.
Your sexual activity will also have a large bearing on which contraceptives are likely to be more practical for you. Do you need additional protection from HIV and other sexual infections? It’s important to remember that hormonal birth control alone will not prevent you from contracting an STI. However, they can be used in tandem with condoms, which are the only way to prevent STIs.
Finally, it’s critical to consider whether you want to have kids in the near future. If not, there are methods that can last for years and some that last indefinitely after only one procedure. If you might want children within the next couple of years, the choice of contraceptive may have some impact on how soon you can conceive after stopping use. For example, if you want kids after coming off hormonal birth control, understand that it may take several months. However, if you want children soon and have a copper IUD, pregnancy may be possible as soon as the device is removed.
Your Health Is an Important Component
It’s also important to consider the limits your health may place on the use of certain birth control methods. You’ll need to consider the potential side effects of a particular contraceptive. Are there minor, manageable inconveniences, or are the effects likely to be more significant for you? We are all unique in that our bodies will respond to the same stimuli differently, and what may be a small downside to one person may be debilitating to another.
You should also consider whether you have any health conditions or predispositions that make a certain method unviable. Alternatively, would a certain contraceptive actually help alleviate what’s afflicting you? Some types of hormonal pills can help people regulate irregular or heavy periods due to polycystic ovary syndrome (PCOS), endometriosis, and other problems. Talking with your healthcare provider can allow you to get clarity on any aspect of birth control you’re unsure about, including helping you answer these questions.
It’s also beneficial to receive a medical professional’s insight into what the ideal type of contraception is for your unique biology, lifestyle, and preferences. They know best how various types of birth control may impact your health or aren’t wise to try at all. You’ll likely find that seeing a gynecologist (a healthcare provider who focuses on women’s sexual health) is a more comfortable or reassuring environment to discuss birth control rather than your general practitioner.
Types of Birth Control Options
Below are the different categories of contraceptives, specific methods/procedures, and their pros and cons.
Non-Hormonal Methods
As mentioned, there are many misconceptions about contraceptives. One is that the Pill and condoms are the predominant methods used for birth control. In fact, IUDs and implants have been on the rise in recent years, so it’s important to remember that everyone’s needs and what’s accessible will differ.
Most non-hormonal birth control methods are barrier methods that work by preventing sperm from reaching/fertilizing the egg. There are also some more involved, long-term types of contraception ranging in degree of invasiveness, such as IUDs and getting your tubes tied. Only condoms can prevent STIs.
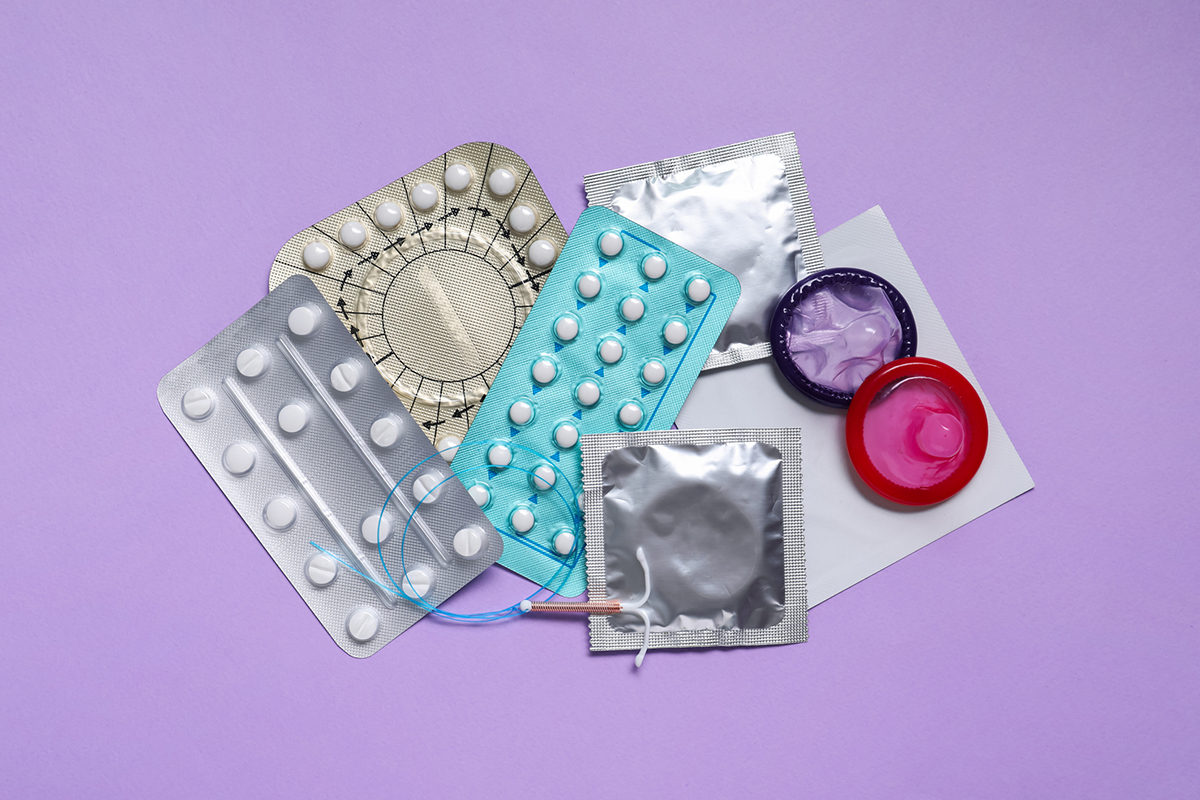
Types of Barrier Birth Control
Condoms
Male condoms are thin coverings made of either latex, plastic, or lambskin. They are used externally and cover the male penis.
Female condoms are lubricated plastic tubes with flexible rings at either end, with one end closed. These are used internally and are inserted into the vagina.
Both are widely available in stores, cost-effective, and up to 85% and 79% effective, respectively. Both prevent semen from entering the uterus and must be used every time sexual intercourse takes place. Male condoms provide very effective STI protection, while female condoms may provide some.
Spermicide
Spermicide is a gel that prevents sperm from reaching the egg. It can be used alone (70% effective) or with an external condom, diaphragm, or cervical cap (94% effective). It must be used each time you have intercourse and is available at most drugstores or with a prescription (up to $270).
Diaphragm/Cervical Cap/Sponge
Diaphragms, cervical caps, and contraceptive sponges are all inserted vaginally, to be used every time (up to 88% effective). Sponges, available in most drugstores, contain spermicide. Diaphragms/caps are flexible cups designed to be used with spermicide and require a provider to determine the appropriate size for you.
Other Types of Non-Hormonal Contraceptives
Copper IUDs
A copper intrauterine device (IUD) is a small, T-shaped piece of copper-wrapped plastic to be inserted once by a provider when prescribed (if not covered by insurance, costs up to $1300). It can last up to 10 years and is low-maintenance.
They work by releasing a small amount of copper that causes a mild inflammatory response that prevents sperm from fertilizing the egg. IUDs are unnoticeable when placed correctly. They are very effective (up to 99%) and, upon wanting to conceive, easily removable. They can also be used as an emergency contraceptive when placed within five days of unprotected sex.
A common concern is they may get lost or tear your uterus; while possible, it’s rare and unlikely. Some IUDs can expel or cause a benign perforation in the uterus upon insertion but only occur in 2-10% and 0.10% of users, respectively.
Fertility Awareness/Natural Family Planning
Also called the natural rhythm, or calendar, method, this refers to tracking your cycle to learn which days pregnancy is more likely (ovulation). Then, you can abstain from sex or use other birth control.

This plan is relatively inexpensive, has no side effects, and works best for those with regular periods. However, it isn’t nearly as effective (75-88%) as other methods. Ovulation home test kits and fertility monitors can help.
Permanent Birth Control/Sterilization
Male vasectomies and female tubal ligations are very effective (99%) and permanent. Depending on insurance, the procedure may be covered or cost up to $1,000 or $6,000, respectively.
Hormonal Contraceptives
Most hormonal contraceptives use the female hormones progestin and estrogen. They work by preventing the ovaries from releasing an egg each month and causing other changes that lower the chances of pregnancy. Long-term and short-term options are available depending on individual preferences. Using them alone will not protect you or your partner from STIs, but using them in tandem with condoms can help you achieve additional protection.
Misconceptions and Myths
A common birth control myth is that hormonal contraceptives will unbalance your natural hormones and cause adverse effects on your mood. However, since the hormones in birth control are very similar to those already found in women’s bodies, stress is more likely to affect your hormones than contraceptives. If you’re concerned about hormones, a potential option could be a copper IUD over one that utilizes hormone release.
Another pervasive worry is that hormonal options can cause cancer, but there is no evidence supporting this. In fact, some hormonal options may actually reduce the risk of ovarian or uterine cancer. Similarly, the misconception that birth control will harm your fertility or the ability to have kids in the future is also inaccurate; hormonal contraceptives are unlikely to affect your ability to conceive beyond your body’s natural ability. This is why women can get pregnant if they miss several pills. The majority of birth control options are entirely reversible.
Another common misconception about hormonal birth control, specifically, is that it will make you gain weight. The truth is that each type of birth control has a different effect on your body, and nobody’s experience is universal. Researchers have yet to find a direct correlation between hormonal contraceptive usage and weight gain. Many women begin using birth control during a time when their body is already naturally gaining weight and changing overall, so it can be hard to know whether the contraceptive is a contributing factor or not.

The birth control shot may increase a person’s appetite, so there may be a potential for weight gain. Still, as with most lifestyle changes, a healthy diet and regular exercise can help you feel more regulated. Low-maintenance birth control methods like hormonal IUDs and the implant contain progestins, which are not known to cause weight gain.
Long-Acting Reversible Contraceptives (LARCs)
Hormonal IUDs
hese are much the same as copper IUDs, including the benefits, but instead release a small amount of progestin to prevent pregnancy (99% effective). They can last from three to eight years, depending on the type. Potential side effects may include irregular, heavy, and/or painful periods.
Birth Control Implant
A small rod is placed under the skin by a provider when prescribed, lasting up to three years. It releases progestin, is very effective (99%), low-maintenance and costs up to $2200 when not covered by insurance. Potential side effects include irregular bleeding, period loss, sore breasts, and headaches.
Short-Acting Hormonal Methods
Pills
Prescribed pills must be taken consistently at the same time every day for maximum effectiveness (93%). They take about a month to take effect, but onwards, they provide constant protection, even during your period or when forgetting a pill. It may cost up to $50, depending on insurance. Lower-hormone mini-pills are also available to help prevent side effects. Other benefits include lighter and/or regulated periods, less cramping, reduced acne, and minimal PMS. Side effects can include temporary breast tenderness, nausea, headaches, and period irregularity. Those containing estrogen also increase the risk of blood clots.
Hormonal Patch
The patch is worn on the skin and releases hormones to be absorbed. It must be replaced weekly with one week off monthly. Its effectiveness (93%) is dependent on consistent use, and it may cost up to $150.
Shot/Injection
The shot can be administered by a doctor/nurse every three months when prescribed. The progestin contained in the shot prevents ovulation and prevents sperm from reaching the egg by thickening cervical mucus. Shots are 96% effective and cost up to $150.
Hormonal Ring
Vaginal rings are inserted into the vagina and release hormones that prevent pregnancy. They require a prescription and are to be replaced monthly, some lasting longer than others. These are 91% effective and, depending on insurance, may cost up to $200.
Emergency Contraception Pills (ECPs)
Also called the morning-after pill or Plan B, this birth control option can be provided over-the-counter or as prescribed. It is most effective (90%) soon after unprotected sex but may be effective for up to five days afterward.
ECPs are meant to be used when another contraceptive malfunctions or is forgotten. They are not designed for regular use, as taking them routinely can render them less effective. If you are already pregnant or become pregnant despite taking the ECP, it will not cause harm.
Trust Arizona Gynecology Consultants for Your Birth Control Needs

If you are searching for the ideal contraceptive for your needs, it’s critical to consider all the factors listed above. To ensure you find the best fit for you, schedule an appointment with a trusted gynecologist. Our AZGYN team can help you narrow down the options, provide you with professional advice from our extensive experience, and write a prescription as needed. Schedule an appointment today.
Sources:
- Kaiser Family Foundation. (2022, November 3). Contraception in the United States: A closer look at experiences, preferences, and coverage. Retrieved from https://www.kff.org/womens-health-policy/report/contraception-in-the-united-states-a-closer-look-at-experiences-preferences-and-coverage/
- Office of Disease Prevention and Health Promotion. (n.d.). Choose the right birth control. Health.gov. Retrieved from https://health.gov/myhealthfinder/healthy-living/sexual-health/choose-right-birth-control
- Office on Women’s Health. (n.d.). Birth control methods. Women’s Health. Retrieved from https://www.womenshealth.gov/a-z-topics/birth-control-methods
- Centers for Disease Control and Prevention. (n.d.). Contraceptive use. Retrieved from https://www.cdc.gov/nchs/fastats/contraceptive.htm
- Nationwide Children’s Hospital. (2011). Birth Control Myths. Nationwidechildrens.org. https://www.nationwidechildrens.org/specialties/bc4teens/resources/birth-control-myths

